 They also found progressive intra-articular displacement both preoperatively and postoperatively and recommend close radiographic follow-up of these fractures. J Pediatr Orthop 34:144–149, 2014) found most patients required open reduction through a dorsal approach to the MTP joint and often found a periosteal flap of tissue in the physis which prevented a successful closed reduction. The toe may be fitted with a splint to keep it in a fixed. #Non displaced toe fracture seriesAnother case series with ten patients published in 2014 (Kramer et al. Sometimes rest is all that is needed to treat a traumatic fracture of the toe. A case series with four gymnasts with Salter-Harris (SH) III and IV injuries that all underwent open reduction and pin fixation with good outcomes has also been described (Perugia et al. Most of these fractures are Salter-Harris III or IV injuries. The foot also contains sesamoid bones (bones embedded within a tendon). This means the line of the break goes all the way through your bone. Forefoot: 5 metatarsals and 14 phalanges. fracture: Nonweight-bearing cast for 6 to 8. Unstable, displaced phalanx fractures require surgical management, preferably via closed reduction and percutaneous pinning. Stable, reduced phalanx fractures are immobilized but require close monitoring to ensure maintenance of fracture reduction. If the patient is too symptomatic in the soft. Nondisplaced phalanx fractures are managed with splint immobilization. You might see oblique fractures referred to as complete fractures. Referral is generally indicated for intra-articular or displaced metatarsal fractures. They happen when one of your bones is broken at an angle. What is an oblique fracture Oblique fractures are a type of broken bone. Reduction is recommended if the great toe proximal phalanx joint surface is displaced more than 2–3 mm or 25% of the joint surface is involved. Overview An oblique fracture angles across a bone. Displaced intra-articular fractures in older children can be treated often with closed reduction, open reduction if needed, and percutaneous pin or screw stabilization for 4–6 weeks. A case series of hallux fractures found that soccer was the most common mechanism and 86% of children were treated non-operatively (Petnehazy et al. A type 2 excludes note indicates that the condition excluded is not part of the condition it is excluded from but a patient may have both conditions at the same time. A common treatment regimen is weight-bearing as tolerated often in a stiff-soled shoe until the patient is comfortable ambulating in their regular shoes. A type 2 excludes note represents 'not included here'. Treatment of most of these injuries is non-operative with symptomatic treatment. Displaced fractures (or for any fractures involving the great toe) - Fracture clinic within 7 days. This article highlights the different types of splints and casts that are used in various circumstances and how each is applied.Phalanx fractures of the toes are fairly rare injuries in children. toe fractures include open or closed, extra-articular or intra-articular fractures of the first toe (hallux/great) and second to fifth (lesser) toes. Nondisplaced fractures of the other toes do not require specific follow-up. #Non displaced toe fracture fullIndications and accurate application techniques vary for each type of splint and cast commonly encountered in a primary care setting. A severe fracture will limit motion due to swelling and pain, but a non-displaced single fracture of most bones of the foot and ankle will allow full motion. Selection of a specific cast or splint varies based on the area of the body being treated, and on the acuity and stability of the injury. All patients who are placed in a splint or cast require careful monitoring to ensure proper recovery. Excessive immobilization from continuous use of a cast or splint can lead to chronic pain, joint stiffness, muscle atrophy, or more severe complications (e.g., complex regional pain syndrome). To maximize benefits while minimizing complications, the use of casts and splints is generally limited to the short term. 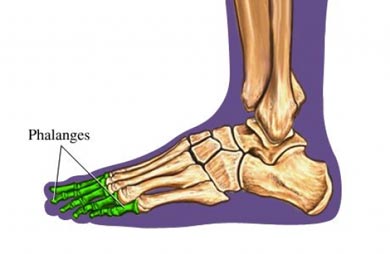
Recovery can be long, and side effects are common. Some fractures require surgery to repair. A patella fracture can be simple or complex. It’s usually caused by a traumatic injury, such as a fall or a blow to your kneecap. 
Because of this, casts provide superior immobilization but are less forgiving, have higher complication rates, and are generally reserved for complex and/or definitive fracture management. A patella fracture is a break in your kneecap, the bone that covers your knee joint. 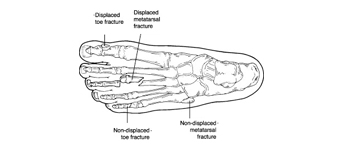
This quality makes splints ideal for the management of a variety of acute musculoskeletal conditions in which swelling is anticipated, such as acute fractures or sprains, or for initial stabilization of reduced, displaced, or unstable fractures before orthopedic intervention. Splints are noncircumferential immobilizers that accommodate swelling. Management of a wide variety of musculoskeletal conditions requires the use of a cast or splint. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
